CNN
—
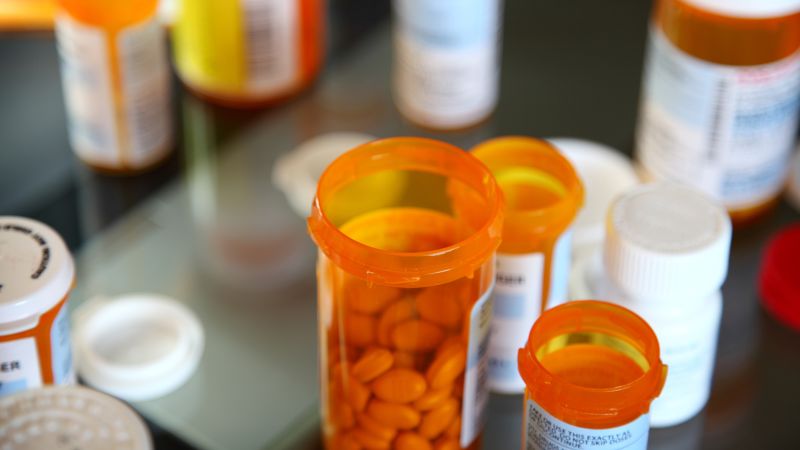
The Biden administration unveiled Tuesday the names of the first 10 drugs subject to price negotiations in Medicare, including blood thinners and diabetes medications.
They are: Eliquis, Jardiance, Xarelto, Januvia, Farxiga, Entresto, Enbrel, Imbruvica, Stelara, and Fiasp and certain other insulins made by Novo Nordisk, including NovoLog.
The medications treat heart disease, certain cancers, diabetes and autoimmune diseases. Medicare enrollees currently spend thousands of dollars on these drugs, according to the Department of Health and Human Services.
Once set, the negotiated prices take effect in 2026 – though the drug industry has filed multiple lawsuits seeking to derail the effort. Currently, some patients spend thousands of dollars out of pocket on these medications.
These drugs accounted for $50.5 billion, or about 20%, in total Part D gross covered prescription drug costs, between June 1, 2022, and May 31, 2023, which is the period used to determine which drugs were eligible for negotiation, according to HHS.
The controversial program was authorized by the Inflation Reduction Act that Democrats pushed through Congress last year. The drug industry and their supporters, however, are determined to quash the effort, filing at least eight lawsuits in recent weeks declaring it unconstitutional.
Undaunted, the Centers for Medicare and Medicaid Services has forged ahead with its historic new power, which Democrats have long argued is a way to lower drug prices.
President Joe Biden is set to speak on the initiative Tuesday afternoon, along with his other efforts to lower health care costs. The Inflation Reduction Act also caps the monthly cost of insulin at $35 for Medicare enrollees, allows seniors to get more vaccines at no charge and penalizes drugmakers that raise prices higher than inflation. Other provisions kick in in coming years.
The initial set of drugs was chosen from the top 50 eligible Part D drugs that have the highest total expenditures in Medicare. Only medications that have been on the market for several years without competition are eligible.
CMS will consider multiple factors when developing its initial offer, including the drugs’ clinical benefits, the price of alternatives, research and development costs and patent protection, among others.
Drugmakers have a month to decide whether to participate. CMS and the manufacturers will then negotiate, and the agency will publish the agreed-upon maximum fair prices by September 1, 2024.
If drugmakers don’t comply with the process, they will have to pay an excise tax of up to 95% of the medications’ US sales or pull all their products from the Medicare and Medicaid markets. The pharmaceutical industry contends that the true penalty can be as high as 1,900% of sales.
After the initial round, the Health and Human Services secretary can negotiate another 15 drugs for 2027 and again for 2028. The number rises to 20 drugs a year for 2029 and beyond.
In the first two years of negotiations, CMS will select only Part D drugs that are purchased at pharmacies. It will add Part B drugs, which are administered by doctors, to the mix for 2028.
The program is expected to save Medicare $98.5 billion over 10 years, according to the Congressional Budget Office.
The extent of the savings remains to be seen, with the pharmaceutical industry arguing that many of the medications on the list already have large rebates and discounts due to negotiations that currently occur in Part D insurance plans.
But some experts say Medicare’s new power will make a difference.
“It’s pretty obvious that there are huge savings to be had here, for even a small number of drugs,” said Dr. Benjamin Rome, a health policy researcher at Brigham and Women’s Hospital and Harvard Medical School.
While he said it’s harder to pin down the extent of the savings for Medicare enrollees taking the drugs on the list, Rome noted that the overall savings can help lower premiums and reduce the amount of taxpayer support needed for Medicare.
Advocates also cheered the unveiling of the list.
“The number one reason seniors skip or ration their prescriptions is because they can’t afford them. This must stop,” said Nancy LeaMond, chief advocacy and engagement officer for AARP. “Allowing Medicare to negotiate prices for these first 10 drugs will finally bring much needed access and relief to American families, particularly older adults. We cannot overstate how monumental this law is for older Americans’ financial stability and overall health.”
Manufacturers, however, hope to halt the negotiation process, filing multiple lawsuits in federal courts across the US. They each contend that the program is unconstitutional in various ways.
Many of the drugs on the list are made by pharmaceutical companies that are suing the administration. They include: Eliquis, a blood thinner manufactured by Bristol Myers Squibb; Januvia, a diabetes drug made by Merck; Imbruvica, a leukemia drug made by Janssen Pharmaceuticals, which is owned by Johnson & Johnson; Xarelto, a blood thinner marketed in the US by Janssen; and Jardiance, made by Boehringer Ingelheim.
Among the arguments are that the program violates the Fifth Amendment’s “takings” clause because it allows Medicare to obtain manufacturers’ patented drugs, which are private property, without paying fair market value under the threat of serious penalties.
Plus, the negotiations process violates the First Amendment, the challengers say, because it coerces manufacturers into saying that they agree to the price that the government has dictated and that it’s fair.
Another argument is that the process violates the Eighth Amendment by levying an excessive fine if drugmakers refuse to negotiate and continue selling their products to the Medicare market.
PhRMA, the drug industry’s main lobbying group, said that Tuesday’s announcement “is the result of a rushed process focused on short-term political gain rather than what is best for patients.”
“Giving a single government agency the power to arbitrarily set the price of medicines with little accountability, oversight or input from patients and their doctors will have significant negative consequences long after this administration is gone,” the group said in a statement, adding that the White House’s Cancer Moonshot, an important initiative for Biden, will be hobbled by the harm done to innovation.
In a blog post last week, PhRMA contended that seniors may not benefit and could see their access to their medicines restricted by their Part D drug insurance plans. Also, it said the program ignores the current savings from negotiation and competition that exist in the Part D benefit. And finally, it said the program will curtail research and investment in future drug development.
The CBO estimates that only about 15 fewer drugs would be introduced over the next 30 years, but the pharmaceutical industry argues the true number would be much higher.
The US Chamber of Commerce, which also filed a lawsuit and is seeking a preliminary injunction to halt the process, called the White House’s celebration “premature.”
“The scheme that they are implementing is under a significant cloud of legal uncertainty,” said Neil Bradley, the chamber’s chief policy officer. “All of this could be unwound on the basis that the fundamental program is unconstitutional, and that in the implementation, they’re violating the Administrative Procedures Act.”
The Biden administration, however, has said that nothing in the Constitution bars it from negotiating drug prices. Legal experts have generally agreed.
“The Biden-Harris Administration isn’t letting anything get in our way of delivering lower drug costs for Americans,” Secretary of Health and Human Services Xavier Becerra said in a statement in June. “Pharmaceutical companies have made record profits for decades. Now they’re lining up to block this Administration’s work to negotiate for better drug prices for our families. We won’t be deterred.”
This story has been updated with additional information.